Understanding and Preventing Iliotibial Band Syndrome
At Arduua Trail Running Coaching, we’re dedicated to empowering runners with the knowledge and tools to overcome common challenges and excel in their trail running pursuits.
Iliotibial Band Syndrome (ITBS) is a prevalent issue among runners, and understanding its causes and prevention strategies is essential for maintaining peak performance on the trails.
Iliotibial band syndrome (ITBS) is the second most common knee injury, and is usually associated with long distance running, cycling and weight-lifting.
In this article you will get som info about it, and also some tips and advices how to prevent it, and how to stretch and reduce the stiffness. Check out my personally recorded video in the end of the article!
What is ITBS?
Iliotibial Band Syndrome (ITBS) is a leading cause of knee pain among runners, often attributed to inflammation of the iliotibial band—a thick band of tissue that runs along the outside of the thigh, from the hip to the shin. This inflammation typically occurs due to friction between the IT band and the lateral femoral epicondyle, leading to discomfort and limited mobility, particularly on the outer side of the knee.
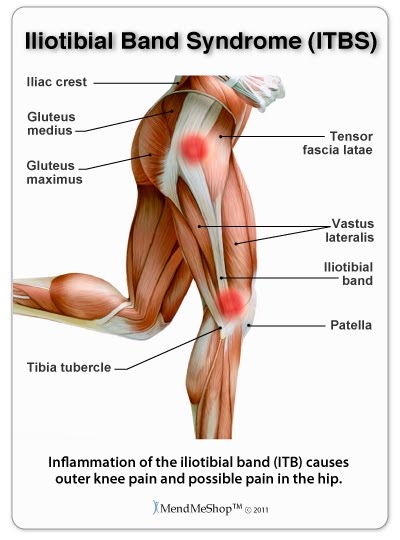
Causes and Risk Factors:
ITBS is commonly associated with activities that involve repetitive knee bending, such as distance running, cycling, and weight-lifting. Runners are particularly susceptible to ITBS, especially when training on uneven terrain or increasing mileage too rapidly. Other risk factors include muscle imbalances, poor running form, and inadequate warm-up or cool-down routines.
Iliotibial band syndrome is one of the leading causes of lateral knee pain in runners. The iliotibial band is a thick band of fascia on the lateral aspect of the knee, extending from the outside of the pelvis, over the hip and knee, and inserting just below the knee. The band is crucial to stabilizing the knee during running, as it moves from behind the femur to the front of the femur during activity. The continual rubbing of the band over the lateral femoral epicondyle combined with the repeated flexion and extension of the knee during running may cause the area to become inflamed.
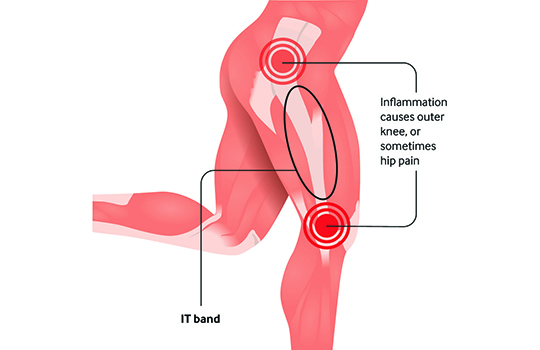
Causes and Risk Factors
ITBS is commonly associated with activities that involve repetitive knee bending, such as distance running, cycling, and weight-lifting. Runners are particularly susceptible to ITBS, especially when training on uneven terrain or increasing mileage too rapidly. Other risk factors include muscle imbalances, poor running form, and inadequate warm-up or cool-down routines.
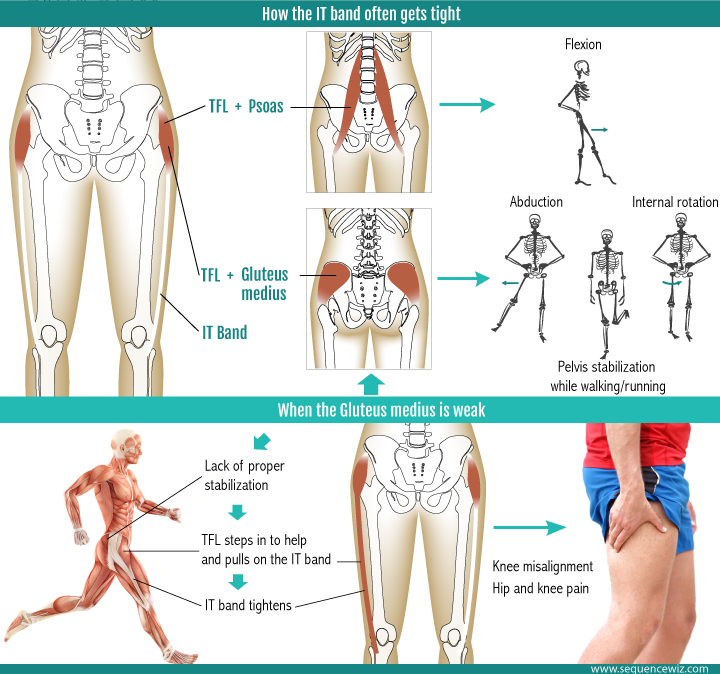
Prevention Strategies
At Arduua, we emphasize a proactive approach to injury prevention, focusing on strengthening key muscles, improving flexibility, and optimizing training techniques. Here are some strategies to help prevent ITBS:
Strengthening Exercises: Target the muscles surrounding the hips, thighs, and knees to improve stability and reduce strain on the IT band. Incorporate exercises such as hip abductions, side leg lifts, and squats into your routine.
Flexibility Training: Regular stretching of the IT band, hip flexors, and quadriceps can help maintain optimal range of motion and prevent tightness that may contribute to ITBS. Foam rolling and self-myofascial release techniques can also be beneficial for loosening tight muscles.
Gradual Progression: Avoid sudden increases in training volume or intensity, as this can place excessive stress on the IT band and increase the risk of injury. Gradually build up mileage and incorporate rest days into your training schedule to allow for adequate recovery.
Proper Equipment: Ensure that your running shoes are appropriate for your foot type and running gait, as improper footwear can exacerbate biomechanical issues that contribute to ITBS. Consider consulting with a specialist to determine the best shoe for your individual needs.
Technique Refinement: Pay attention to your running form and stride mechanics, aiming for a balanced and efficient movement pattern that minimizes excessive lateral movement of the knee. Work with a coach or physical therapist to address any biomechanical issues that may predispose you to ITBS.
By implementing these preventive measures and prioritizing injury awareness, runners can minimize the risk of ITBS and maintain optimal performance on the trails. Remember, prevention is key to long-term success in trail running.
Exercises Videos
In below videos are some of the exercises for strengthening the muscles of the gluteus and legs, without weights, and a few examples of stretching. If you need more tips and suggestions for exercises, you can contact us on our instagram and facebook pages.
Arduua Trail Running Coaching
Your partner in trail running, injury prevention, and performance enhancement
At Arduua, we’re committed to supporting runners of all levels in achieving their goals and staying injury-free. Our experienced coaches provide personalized training plans, expert guidance, and ongoing support to help you reach your full potential on the trails.
Whether you’re training for your first trail race or aiming to improve your performance in ultra marathons, Arduua Trail Running Coaching is here to help. Visit our website to learn more about our coaching services and how we can support your trail running journey.
Don’t let ITBS derail your training and aspirations. Take proactive steps to prevent injury and optimize your performance with Arduua Trail Running Coaching by your side.
Get Support for Your Training
With Arduua Online Coaching, you’ll receive personalized coaching tailored to Trail running Our expert coaches are here to guide you in reaching your full potential and achieving your goals.
If you have any questions, please feel free to reach out to Katinka Nyberg at katinka.nyberg@arduua.com.
Best of luck with your training!
/Arduua Team


